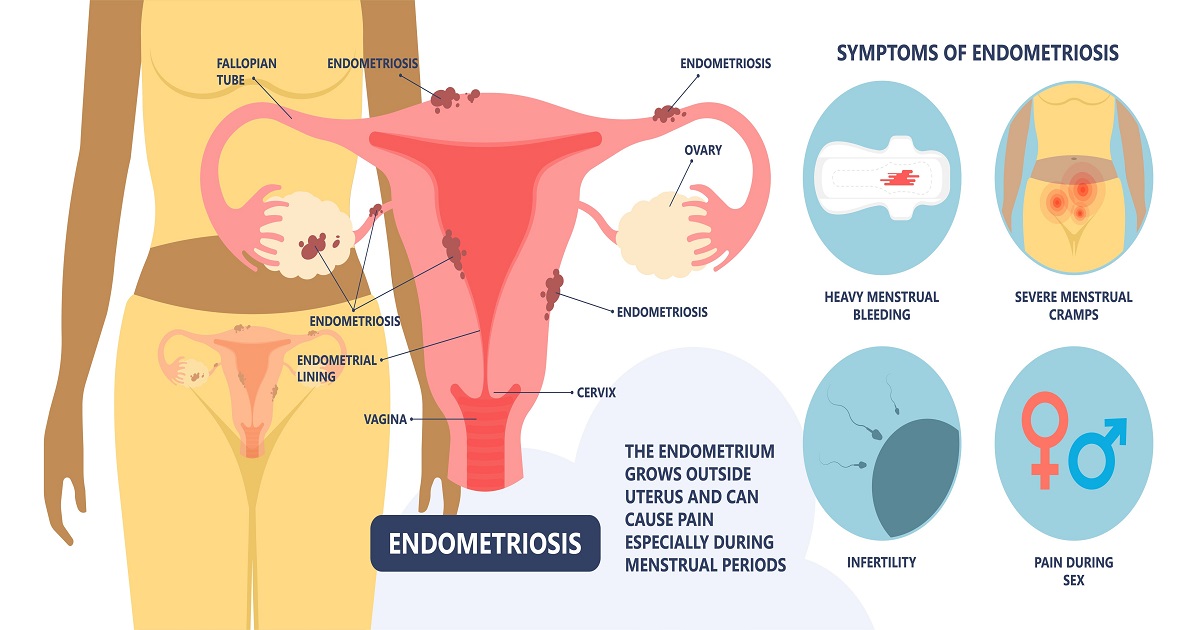
What is Endometriosis: Symptoms & Treatment
IVF IN ENDOMETRIOSIS:
Endometriosis affects millions of women worldwide and can cause a wide range of symptoms, including pelvic pain, heavy menstrual bleeding, and infertility. In fact, approximately 30% to 50% of women with endometriosis may experience difficulty conceiving. This is where in vitro fertilization (IVF) comes in as a possible solution. In this Blog, we will provide a comprehensive guide on IVF in endometriosis, including how it works, its success rates, and potential risks.
WHAT IS ENDOMETRIOSIS?
Endometriosis is a medical condition that affects women during their reproductive years. It occurs when the tissue that normally lines the inside of the uterus, called endometrial tissue, grows outside of the uterus, often in the pelvic region. This misplaced tissue can cause a range of symptoms and complications, including chronic pelvic pain, painful periods, and fertility problems. The exact cause of endometriosis is unknown, but factors such as genetics, hormonal imbalances, and immune system dysfunction may play a role. Treatment options include pain medications, hormonal therapies, and surgery, and lifestyle changes may also help alleviate symptoms. While there is currently no cure for endometriosis, many women are able to find relief from their symptoms with proper management and care.
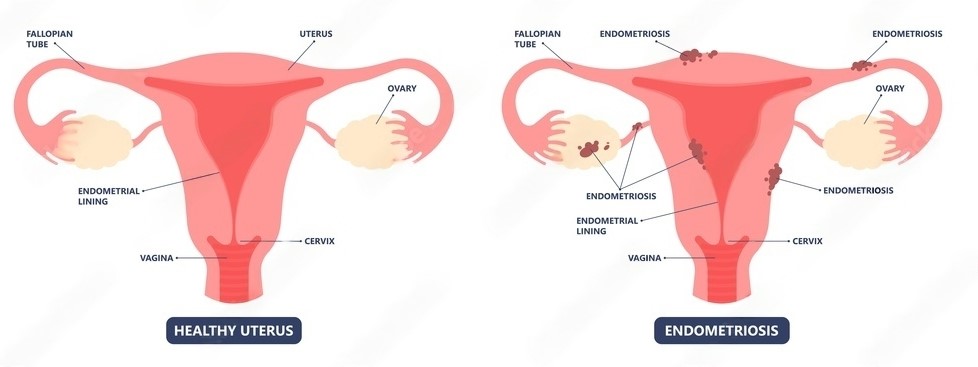
ENDOMETRIOSIS CAUSES:
Here are five key factors that may contribute to the development of endometriosis:
- RETROGRADE MENSTRUATION: This occurs when menstrual blood containing endometrial cells flows back through the fallopian tubes and into the pelvic cavity, where the cells can implant and grow.
- GENETICS: Women who have a family history of endometriosis are at increased risk of developing the condition.
- HORMONAL IMBALANCES: Abnormal levels of estrogen or other hormones in the body may contribute to the development of endometriosis.
- IMMUNE SYSTEM DYSFUNCTION: An immune system that is not functioning properly may allow endometrial cells to implant and grow outside of the uterus.
- ENVIRONMENTAL FACTORS: Exposure to toxins, such as dioxins and PCBs, may increase the risk of developing endometriosis.
It’s worth noting that while these factors may contribute to the development of endometriosis, the exact cause of the condition is not fully understood and may involve a combination of different factors.
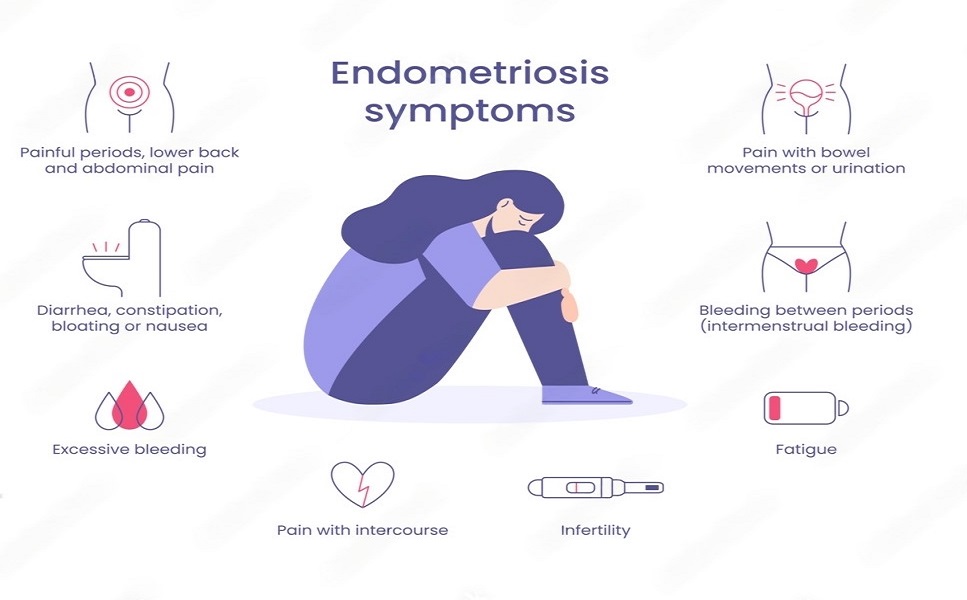
ENDOMETRIOSIS SYMPTOMS:
- Chronic pelvic pain, including severe menstrual cramps and pain during or after sex.
- Heavy or irregular menstrual bleeding.
- Fatigue, nausea, diarrhoea, constipation, or bloating, particularly during menstruation.
- Difficulty getting pregnant or infertility.
- Experience of Painful bowel movements or Painful urination during menstruation.
TESTS TO FIND OUT ENDOMETRIOSIS:
Endometriosis is a condition where the tissue that lines the uterus grows outside of it, causing pain and discomfort. There are several tests that can be used to detect endometriosis, including:
- PELVIC EXAM: A pelvic exam can help identify the presence of any lumps, cysts or other abnormalities in the pelvic area. However, endometriosis lesions may not be visible or palpable during a pelvic exam.
- TRANSVAGINAL ULTRASOUND: This test uses sound waves to create images of the reproductive organs. A transvaginal ultrasound can detect endometriotic cysts in the ovaries, but cannot always detect lesions outside of the ovaries.
- MAGNETIC RESONANCE IMAGING (MRI): An MRI uses a powerful magnet and radio waves to create images of the body. An MRI can detect endometriosis lesions and cysts in the pelvis and other areas of the body.
- LAPAROSCOPY: This is the gold standard diagnostic test for endometriosis, and involves a surgical procedure where a small camera is inserted through a small incision in the abdomen. Laparoscopy allows direct visualization of endometriotic lesions and confirmation of the diagnosis.
- BLOOD TEST: Currently, there is no specific blood test that can diagnose endometriosis. However, certain biomarkers such as CA-125 and Anti-Mullerian Hormone (AMH) levels may be elevated in women with endometriosis, though these biomarkers may not be specific to endometriosis and may be elevated in other conditions as well.
Also read: What is Test Tube Baby
THE IMPACT OF ENDOMETRIOSIS ON FERTILITY:
Endometriosis can directly impact a woman’s fertility by causing inflammation and scarring in the reproductive organs, leading to the obstruction of the fallopian tubes or the formation of ovarian cysts. This can prevent the egg from being released from the ovary or from traveling through the fallopian tubes to reach the uterus for fertilization. Additionally, the endometrial tissue outside the uterus can interfere with the implantation of a fertilized egg, leading to a miscarriage. Endometriosis can also indirectly affect fertility by causing hormonal imbalances that disrupt the menstrual cycle, making it more difficult to conceive. Women with endometriosis may have lower levels of progesterone, a hormone necessary for maintaining a pregnancy. They may also have higher levels of estrogen, which can interfere with ovulation.
In Summary, Endometriosis can affect fertility in the following 3 Ways.
- Damaged or blocked fallopian tubes.
- Inflammation or adhesions that can interfere with ovulation or implantation.
- Changes in the Quality of Eggs or Sperm.
ENDOMETRIOSIS TREATMENT:
IVF involves the retrieval of eggs from the ovaries, fertilization with sperm in a laboratory, and transfer of the resulting embryos into the uterus. This bypasses any issues with the fallopian tubes and allows for direct monitoring and control of the fertilization process. Studies have shown that IVF can be an effective treatment for endometriosis-related infertility, with success rates ranging from 35% to 60%. However, success rates may be affected by various factors, such as the severity of endometriosis, the age of the patient, and the quality of the eggs and sperm.
Also Read: How to Get Pregnant Fast
IVF IN ENDOMETRIOSIS RISKS/SIDE EFFECTS:
Like any medical procedure, IVF carries certain risks and potential complications, such as:
- Ovarian hyperstimulation syndrome (OHSS) is a potential complication of IVF in endometriosis, characterized by enlarged ovaries, fluid retention, and abdominal discomfort.
- Endometriosis can affect the quality and quantity of eggs retrieved during IVF, reducing the chances of successful fertilization and implantation.
- Endometrial receptivity may be compromised in women with endometriosis, leading to a lower likelihood of successful embryo implantation and pregnancy.
- Women with endometriosis may have a higher risk of ectopic pregnancy following IVF due to the distorted pelvic anatomy caused by the condition.
- Endometriosis-related inflammation may increase the risk of implantation failure, pregnancy loss, and adverse obstetric outcomes such as preterm birth and low birth weight.
However, with proper monitoring and management, these risks can be minimized.
IVF IN ENDOMETRIOSIS SUCCESS RATES:
Studies show that up to 90% of endometriosis patients experienced relief in endometriosis symptoms and complaints. In addition, over 60% of patients who wished to become pregnant were able to conceive after the surgery. Other studies confirm that pregnancy is likely to be achieved after laparoscopy traetment for endometriosis.
TIPS FOR INCREASING IVF SUCCESS RATES IN ENDOMETRIOSIS PATIENTS:
- Seek treatment from a fertility specialist with experience in treating endometriosis.
- Consider undergoing laparoscopic surgery to remove endometrial tissue before starting IVF.
- Optimize your overall health by maintaining a healthy weight, quitting smoking, and managing any underlying medical conditions.
- Consider using donor eggs or sperm if your own are of poor quality.
- Consider using preimplantation genetic testing to screen for any genetic abnormalities in embryos before transfer.
Also Read:What Is IVF Process/Procedure
IVF can be an effective treatment option for women with endometriosis-related infertility. However, it is important to understand the potential risks and complications, as well as the factors that may affect success rates. Working closely with a fertility specialist can help optimize your chances of a successful IVF outcome.
IVF WITH ENDOMETRIOSIS TREATMENT COST:
The cost of IVF with endometriosis typically ranges from (1.5-2) Lac INR in India i.e. (2-3) K USD. Little Angel IVF Offers Comprehensive Payments Options with 0% Interest Offered by Partnered Banking Institutions.
PLAN YOUR ENDOMETRIOSIS TREATMENT:
Little Angel IVF has a team of experienced doctors and staff who are dedicated to helping patients achieve their dreams of parenthood. Dr Mona Dahiya has over 20 years of experience in treating endometriosis and has helped countless women become pregnant. The Staff is compassionate and supportive, providing patients with the care and attention they need during their treatment.
INDIA’S BEST IVF DOCTOR:
Endometriosis is a painful disorder in which the tissue that lines the uterus grows outside of it. This can cause a range of symptoms, including painful periods, infertility, and even depression. However, with advancements in medical technology, there is hope for women with endometriosis who want to conceive. Little Angel IVF is a leading fertility clinic that offers cutting-edge technology and personalized care for women with endometriosis. Here are just a few reasons why you should consider Little Angel IVF for your IVF treatment.
Little Angel IVF is an excellent choice for women with endometriosis who are looking for personalized, high-quality care for their IVF treatment. With experienced doctors, advanced technology, personalized treatment plans, high success rates, and patient-focused care, Little Angel IVF offers patients the best chance of achieving their dream of parenthood.
FAQs:
Q: Can endometriosis be cured completely?
A: There is no known cure for endometriosis at the present. However, there are various treatments available to manage symptoms and slow the progression of the disease.
Q: What is the best medication for endometriosis?
A: The best medication for endometriosis depends on the individual case and their specific symptoms. Some common medications used to treat endometriosis include nonsteroidal anti-inflammatory drugs (NSAIDs), hormonal contraceptives, and gonadotropin-releasing hormone (GnRH) agonists.
Q: What is the main cause of endometriosis?
A: The exact cause of endometriosis is not fully understood, but it is believed to be a combination of genetic, hormonal, and environmental factors.
Q: How will I know if I have endometriosis?
A: The only way to definitively diagnose endometriosis is through laparoscopic surgery. However, common symptoms of endometriosis include painful periods, pelvic pain, pain during sex, and infertility.
Q: How to prevent endometriosis?
A: There is no known way to prevent endometriosis, but some lifestyle factors may reduce the risk of developing the condition, such as maintaining a healthy weight, avoiding excessive alcohol consumption, and avoiding exposure to environmental toxins.
Q: What are the first signs of endometriosis?
A: The first signs of endometriosis often include painful periods, pelvic pain, and pain during sex. Other symptoms may include fatigue, bloating, and bowel or bladder problems.
Q: How serious is endometriosis?
A: Endometriosis can range from mild to severe, with some individuals experiencing debilitating symptoms and others experiencing no symptoms at all. In some cases, endometriosis can lead to infertility or other complications. It is important to work with a healthcare provider to manage symptoms and monitor the progression of the disease.
Q: Who can get endometriosis?
A: Endometriosis can affect anyone who menstruates, regardless of age or gender. However, it is most commonly diagnosed in individuals between the ages of 25 and 40.
Q: Is endometriosis genetic?
A: There appears to be a genetic component to endometriosis, as it tends to run in families. However, the exact genetic factors involved are not fully understood.
Q: Can endometriosis go away on its own?
A: Endometriosis does not typically go away on its own, but symptoms may improve with treatment. In some cases, symptoms may temporarily improve during pregnancy or menopause.
Q: What happens if endometriosis is left untreated?
A: If left untreated, endometriosis can lead to the formation of scar tissue and adhesion, which can cause chronic pain and lead to infertility. In rare cases, endometriosis may also lead to the development of certain types of cancer.
Q: Can endometriosis be prevented?
A: There is no known way to prevent endometriosis, but maintaining a healthy lifestyle and managing underlying medical conditions may help reduce the risk of developing the condition. Regular pelvic exams and early detection may also help to manage symptoms and prevent complications.
Q: What are the complications of endometriosis?
A: Complications of endometriosis can include chronic pain, adhesion, infertility, ovarian cysts, and in rare cases, cancer.
Q: Can I get cancer from endometriosis?
A: Although rare, there is a slight increased risk of certain types of ovarian cancer in individuals with endometriosis.
Q: Can you still have endometriosis after menopause?
A: Although endometriosis is typically diagnosed during the reproductive years, it is possible to have endometriosis after menopause. Hormone replacement therapy may also cause endometriosis to persist after menopause.
Q: Can you get pregnant if you have endometriosis?
A: It is possible to get pregnant with endometriosis, although the condition can make it more difficult. Treatment may be necessary to improve fertility.
Q: How can I reduce endometriosis naturally?
A: Natural remedies for endometriosis include reducing stress, eating a healthy diet, exercising regularly, and using heat therapy to alleviate pain.
Q: How can I stop endometriosis from growing?
A: Treatment options for endometriosis include hormonal therapies, surgery to remove endometrial tissue, and lifestyle changes to manage symptoms and slow the progression of the disease.
Q: What foods prevent endometriosis?
A: Some foods that may help reduce the risk of endometriosis include fruits, vegetables, whole grains, lean proteins, and omega-3 fatty acids.
Q: What increases risk of endometriosis?
A: Risk factors for endometriosis include a family history of the condition, early onset of menstruation, and prolonged menstrual cycles.
Q: Does endometriosis always come back?
A: Endometriosis has a high rate of recurrence, even after treatment. Regular monitoring and follow-up care is important to manage symptoms and prevent complications.
Q: How quickly can endometriosis come back?
A: Endometriosis can recur as early as a few months after treatment, although the time frame can vary depending on the individual case.
Q: How to prevent endometriosis from coming back?
A: Preventing the recurrence of endometriosis can involve ongoing management of symptoms and monitoring of the disease, as well as lifestyle changes to promote overall health.
Q: How to explain endometriosis pain?
A: Endometriosis pain can range from mild discomfort to severe, debilitating pain. The pain may be associated with menstruation or intercourse, and can also cause pelvic pain, bowel or bladder problems, and fatigue.
Q: How to prevent endometriosis after surgery?
A: Preventing the recurrence of endometriosis after surgery may involve ongoing management of symptoms and regular monitoring of the disease. Hormonal therapies or other treatments may also be recommended to slow the progression of the disease.
Q: What is the best treatment for endometriosis?
A: The best treatment for endometriosis depends on the individual case and the severity of symptoms. Treatment options can include hormonal therapies, surgery to remove endometrial tissue, and lifestyle changes to manage symptoms.
Q: How is endometriosis diagnosed?
A: Endometriosis is typically diagnosed through a combination of medical history, pelvic exams, imaging tests, and sometimes laparoscopic surgery.
Q: Can endometriosis cause fatigue?
A: Yes, endometriosis can cause fatigue as a result of chronic pain, hormonal imbalances, or other associated symptoms.
Q: Is there a cure for endometriosis?
A: While there is no cure for endometriosis, symptoms can be managed and the progression of the disease can be slowed through various treatment options.
Q: Can endometriosis cause digestive problems?
A: Yes, endometriosis can cause digestive problems such as bloating, constipation, or diarrhea due to the close proximity of the endometrial tissue to the intestines.
Q: Can endometriosis cause back pain?
A: Yes, endometriosis can cause back pain as a result of the close proximity of the endometrial tissue to the nerves that supply the back muscles.
Q: How long does it take to recover from endometriosis surgery?
A: Recovery time after endometriosis surgery can vary depending on the individual case and the type of surgery performed. In general, it can take several weeks to a few months to fully recover.
Q: What is the difference between adenomyosis & endometriosis?
A: Endometriosis is the growth of endometrial tissue outside of the uterus, while adenomyosis is the growth of endometrial tissue within the uterine muscle.
Q: Can endometriosis cause infertility?
A: Yes, endometriosis can cause infertility due to the formation of scar tissue and adhesions, as well as hormonal imbalances that can affect ovulation.
Q: Can endometriosis cause depression?
A: Yes, endometriosis can cause depression as a result of chronic pain, hormonal imbalances, or other associated symptoms.