Hydrosalpinx: Symptoms, Causes and Treatment
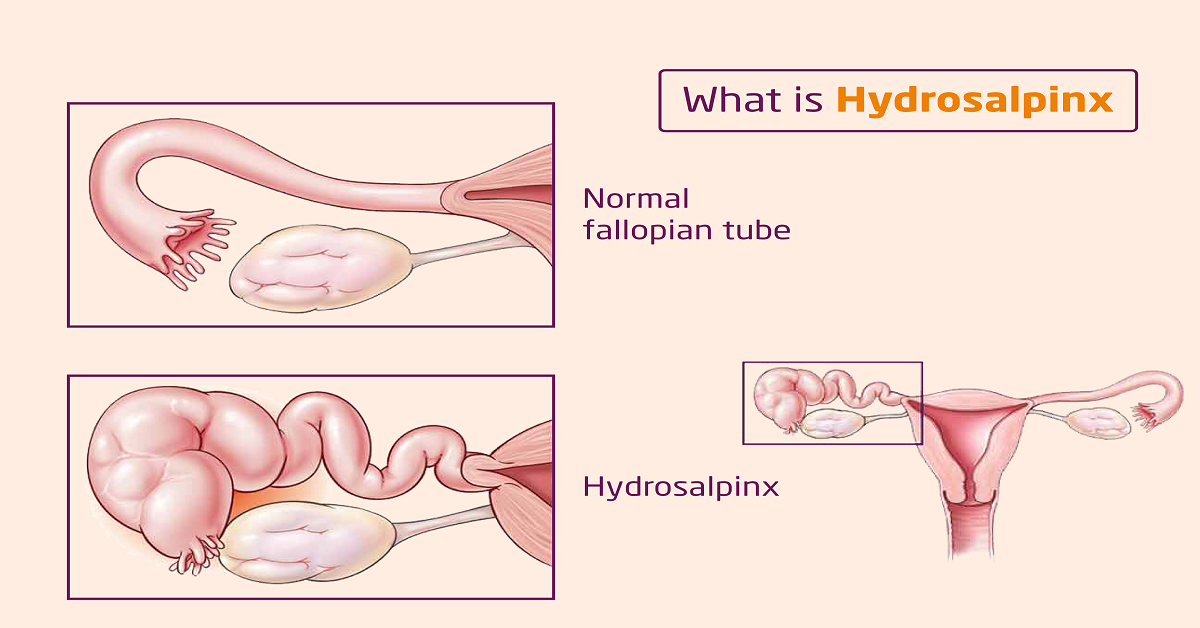
What is Hydrosalpinx?
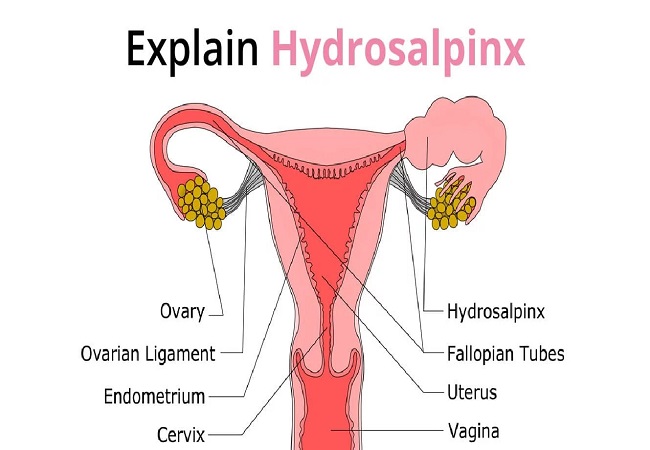
Hydrosalpinx, derived from the Greek words “hydro” (meaning water) and “salpinx” (meaning tube), refers to the accumulation of fluid in the fallopian tubes. These tubes play a vital role in transporting eggs from the ovaries to the uterus. However, when the tubes become blocked or obstructed, fluid can accumulate, leading to the formation of hydrosalpinx.
Symptoms of Hydrosalpinx:
Identifying the symptoms of hydrosalpinx is crucial for early detection and timely treatment. While some women may not experience any symptoms at all, others may notice:
- Pelvic pain: Persistent or intermittent pain in the pelvic region is a common symptom of hydrosalpinx. The severity of the pain can vary from mild discomfort to severe cramping.
- Hydrosalpinx Discharge Color: Some women may notice an abnormal vaginal discharge, which can be thin, clear, or white in color.
- Pain during intercourse: Sexual intercourse may become painful or uncomfortable for women with hydrosalpinx.
- Irregular menstrual cycles: Hydrosalpinx can cause disruptions in the menstrual cycle, leading to irregular periods.
Hydrosalpinx Impact on Fertility
Hydrosalpinx can significantly impact a woman’s fertility. The presence of fluid in the fallopian tubes can hinder the fertilization process by preventing sperm from reaching the egg. It can also interfere with the movement of the fertilized egg toward the uterus, increasing the risk of ectopic pregnancy.
Hydrosalpinx Potential Complications:
If left untreated, hydrosalpinx can lead to several complications:
- Increased risk of infertility: The obstruction caused by hydrosalpinx can prevent successful conception, making it difficult for women to become pregnant naturally.
- Ectopic pregnancy: The presence of fluid in the fallopian tubes increases the likelihood of ectopic pregnancy, where the fertilized egg implants and develops outside the uterus.
- Chronic pelvic pain: Hydrosalpinx can cause persistent pelvic pain, affecting a woman’s quality of life and daily activities.
- Adhesions and scarring: In some cases, the inflammation associated with hydrosalpinx can lead to the development of adhesions or scar tissue, further compromising fertility.
Causes of Hydrosalpinx:
Understanding the underlying causes of hydrosalpinx can help in its prevention and management. Some common causes include:
- Infection and Inflammation: Infections in the reproductive organs, such as pelvic inflammatory disease (PID), can lead to inflammation and scarring of the fallopian tubes. This scarring can eventually result in the formation of hydrosalpinx.
- Pelvic Inflammatory Disease (PID): PID, often caused by sexually transmitted infections, can cause inflammation and damage to the fallopian tubes, increasing the risk of hydrosalpinx.
- Previous Pelvic Surgery or Ectopic Pregnancy: Previous pelvic surgeries, such as surgeries for appendicitis or ovarian cysts, can cause scarring and blockages in the fallopian tubes, leading to hydrosalpinx. Additionally, an ectopic pregnancy, where the fertilized egg implants outside the uterus, can result in damage to the fallopian tubes, increasing the risk of hydrosalpinx.
- Endometriosis: Endometriosis, a condition where the tissue lining the uterus grows outside the uterus, can affect the fallopian tubes, leading to inflammation, scarring, and the development of hydrosalpinx.
- Other Potential Causes: While infection, inflammation, previous surgeries, and endometriosis are common causes of hydrosalpinx, there are other factors that can contribute to its development. These include hormonal imbalances, congenital abnormalities, and certain medical conditions.’
Diagnosis of Hydrosalpinx:
Medical History and Physical Examination
Diagnosing hydrosalpinx typically begins with a comprehensive medical history and physical examination. Your healthcare provider will inquire about your symptoms, menstrual history, sexual activity, and any previous reproductive health issues. Additionally, a pelvic examination will be conducted to assess any signs of tenderness, abnormal discharge, or palpable masses. These initial steps provide valuable insights and help guide further diagnostic procedures.
Imaging Techniques
Imaging techniques play a crucial role in diagnosing hydrosalpinx. Some common imaging methods include:
- Ultrasound: Ultrasound imaging uses high-frequency sound waves to create real-time images of the reproductive organs. It can help visualize the fallopian tubes and identify the presence of fluid-filled structures.
- Hysterosalpingography (HSG): HSG involves the injection of a contrast dye into the uterus, followed by X-ray imaging. This technique allows for the evaluation of the fallopian tubes’ structure and can reveal blockages or abnormalities.
- Transvaginal Ultrasound: This specialized ultrasound technique involves inserting a probe into the vagina to obtain detailed images of the reproductive organs. It provides a closer look at the fallopian tubes and can aid in identifying hydrosalpinx.
- Magnetic Resonance Imaging (MRI): In certain cases, MRI scans may be utilized to visualize the pelvic area and provide a more detailed assessment of the fallopian tubes.
Laparoscopy as a Diagnostic Tool
Laparoscopy is a minimally invasive surgical procedure that may be employed for the diagnosis of hydrosalpinx. It involves making small incisions in the abdomen to insert a thin, lighted instrument called a laparoscope. This allows the doctor to visualize the reproductive organs directly and identify any blockages or fluid accumulation in the fallopian tubes. Laparoscopy not only aids in diagnosis but can also serve as a therapeutic measure by providing an opportunity for surgical intervention if necessary.
Treatment Options for Hydrosalpinx:
Conservative Management for Hydrosalpinx
- Antibiotic Therapy: In cases where hydrosalpinx is caused by infection or inflammation, antibiotic therapy may be prescribed. This treatment aims to eradicate the underlying infection and reduce inflammation in the fallopian tubes. It is essential to follow the prescribed antibiotic regimen diligently and complete the full course of treatment to ensure the effective resolution of the infection.
- Pain Management: Managing pain associated with hydrosalpinx is an integral part of conservative management. Nonsteroidal anti-inflammatory drugs (NSAIDs) may be recommended to alleviate pain and reduce inflammation. Your healthcare provider may suggest appropriate pain management strategies based on your individual needs and preferences.
Lifestyle Changes
Certain lifestyle changes can complement conservative management for hydrosalpinx. These may include:
- Maintaining a Healthy Weight: Being overweight or underweight can impact reproductive health. Achieving and maintaining a healthy weight through a balanced diet and regular exercise can positively contribute to managing hydrosalpinx.
- Quitting Smoking: Smoking has been linked to various reproductive health issues, including damage to the fallopian tubes. Quitting smoking can improve overall fertility and reproductive well-being.
- Stress Management: High levels of stress can affect hormonal balance and reproductive health. Practicing meditation, yoga, or engaging in hobbies can help reduce stress levels and promote well-being.
Surgical Interventions for Hydrosalpinx
- Salpingectomy: Salpingectomy involves the surgical removal of the affected fallopian tube. This procedure is usually considered when the hydrosalpinx is severe, irreparable, or causing significant pain. Salpingectomy may be performed using traditional open surgery or minimally invasive techniques such as laparoscopy. After the affected tube is removed, the remaining healthy fallopian tube can still support natural conception.
- Salpingostomy: Salpingostomy is a surgical procedure that aims to create a new opening in the blocked fallopian tube, allowing the accumulated fluid to drain. This procedure is typically considered for cases where preserving the fallopian tube is desirable, such as when fertility preservation is a priority. Salpingostomy may improve the chances of natural conception, although it is important to note that the success rates vary depending on individual factors.
- Tubal Cannulation: Tubal cannulation is a minimally invasive procedure that involves inserting a catheter or specialized instruments through the cervix and into the fallopian tubes. This procedure is used to clear blockages in the tubes, restore normal tubal function, and improve the chances of natural conception. Tubal cannulation is often performed under imaging guidance, such as hysterosalpingography, to ensure precise placement of the instruments.
- In vitro Fertilization (IVF) with Tubal Bypass: In cases where the fallopian tubes are severely damaged or when other treatment options have been unsuccessful, in vitro fertilization (IVF) with tubal bypass may be considered. IVF involves retrieving eggs from the ovaries, fertilizing them with sperm in a laboratory setting, and transferring the resulting embryos into the uterus. By bypassing the fallopian tubes, IVF offers a direct route for fertilization and increases the chances of achieving a successful pregnancy. This approach is particularly beneficial for individuals with bilateral hydrosalpinx or other underlying fertility issues.
Prevention of Hydrosalpinx:
Preventing hydrosalpinx involves maintaining good pelvic health and taking proactive measures to reduce the risk of infections and inflammatory conditions. Here are some important prevention tips:
Maintaining Good Pelvic Health:
- Practice Good Hygiene: Maintain proper hygiene by regularly washing the genital area with mild soap and water. Avoid using harsh chemicals or perfumed products that may disrupt the natural balance of the vagina.
- Stay Hydrated: Drink an adequate amount of water daily to promote overall health and support the proper functioning of the reproductive organs.
- Eat a Balanced Diet: A nutritious diet rich in fruits, vegetables, whole grains, and lean proteins provides essential nutrients that contribute to pelvic health.
- Exercise Regularly: Engage in regular physical activity to promote blood circulation and strengthen pelvic muscles.
Practicing Safe Sex and Avoiding Sexually Transmitted Infections
- Use Barrier Methods: Consistently use barrier methods such as condoms during sexual intercourse to reduce the risk of sexually transmitted infections (STIs) that can lead to pelvic inflammatory disease (PID) and subsequent hydrosalpinx.
- Get Tested for STIs: Regularly undergo STI screenings, especially if you have multiple sexual partners or engage in high-risk behaviors. Early detection and treatment of STIs can prevent the development of pelvic infections.
Prompt Treatment of Infections and Inflammatory Conditions
- Seek Medical Attention: If you experience any symptoms of pelvic infections or inflammatory conditions, such as pelvic pain, abnormal discharge, or fever, seek prompt medical attention. Timely treatment can prevent the spread of infection and potential damage to the fallopian tubes.
- Complete Prescribed Medications: If you are diagnosed with an infection or inflammatory condition, follow your healthcare provider’s instructions and complete the full course of prescribed medications. This helps eradicate the infection and reduce the risk of complications.
- Manage Chronic Conditions: If you have chronic conditions such as endometriosis or previous pelvic surgeries, work closely with your healthcare provider to manage these conditions effectively. Regular monitoring and appropriate treatment can minimize the risk of hydrosalpinx development.
Can Hydrosalpinx Burst/Rupture?
Hydrosalpinx itself does not typically burst. However, the accumulation of fluid in the fallopian tubes can exert pressure, potentially leading to complications such as tubal rupture or leakage. Rupture is more common in cases of severe hydrosalpinx or if the underlying cause, such as infection or inflammation, is left untreated. Rupture can cause severe abdominal pain and requires immediate medical attention. If you experience intense pain or suspect a rupture, seek prompt medical care.
Hydrosalpinx Rupture Symptoms
When a hydrosalpinx ruptures, it can manifest with distinct symptoms. These may include:
- Severe Abdominal Pain: The rupture of a hydrosalpinx often results in sudden and intense abdominal pain. The pain may be localized or spread throughout the lower abdomen. It is essential to differentiate this pain from other causes and seek medical evaluation to determine the underlying cause and provide appropriate treatment.
- Nausea and Vomiting: Rupture can lead to feelings of nausea and may be accompanied by vomiting. These symptoms are often associated with severe pain and should not be ignored.
- Shoulder Pain: In some cases, shoulder pain may be present. This occurs due to the irritation of the diaphragm by the fluid released from the ruptured hydrosalpinx. If you experience shoulder pain along with severe abdominal pain, it could indicate a ruptured hydrosalpinx.
If you experience any of these symptoms or suspect a rupture, seek immediate medical attention to receive a proper diagnosis and appropriate treatment.
Hydrosalpinx and Cancer Risk
Hydrosalpinx itself does not increase the risk of developing cancer in the fallopian tubes. However, it is important to note that chronic inflammation and underlying conditions that can cause hydrosalpinx, such as pelvic inflammatory disease (PID) or endometriosis, may carry their own potential cancer risks. It is crucial to discuss any concerns with your healthcare provider to understand the specific risks associated with your individual situation.
Can Hydrosalpinx Go Away on Its Own?
In some cases, small hydrosalpinx may resolve on its own without treatment. However, it is important to remember that larger or more severe hydrosalpinx are less likely to resolve spontaneously. Additionally, untreated hydrosalpinx can lead to complications and worsen over time. Therefore, it is essential to consult with a healthcare professional for an accurate diagnosis and appropriate treatment plan.
Conclusion
Hydrosalpinx is a condition that requires medical attention and proper treatment. With advancements in medical technology and reproductive techniques, there is hope for women affected by hydrosalpinx to achieve their dreams of starting a family. By raising awareness, promoting early detection, and ensuring access to appropriate medical care, we can empower women to take control of their reproductive health and overcome the challenges posed by hydrosalpinx.
F.A.Q
Q: What is the treatment for hydrosalpinx?
A: The primary treatment for hydrosalpinx is surgical intervention, typically in the form of laparoscopic or open surgery. The surgical options include salpingectomy (removal of the affected fallopian tube) or salpingostomy (creation of an opening in the tube to drain the fluid). In some cases, fertility-preserving surgeries such as tubal reanastomosis or fimbrioplasty may be considered.
Q: What are the symptoms of hydrosalpinx?
A: Hydrosalpinx, a condition characterized by the blockage and accumulation of fluid in the fallopian tubes, may present with various symptoms. Common symptoms include pelvic pain or discomfort, lower abdominal pain, unusual vaginal discharge, and irregular menstrual cycles. However, some individuals with hydrosalpinx may not experience any noticeable symptoms.
Q: Is hydrosalpinx painful?
A: Yes, hydrosalpinx can cause pelvic pain or discomfort. The presence of fluid-filled fallopian tubes can lead to distention, inflammation, and pressure on surrounding tissues, resulting in pain. However, it’s important to note that not all individuals with hydrosalpinx experience pain, and the severity of pain can vary among individuals.
Q: Is it possible to get pregnant with hydrosalpinx?
A: It can be challenging to conceive naturally with hydrosalpinx, as the blocked or damaged fallopian tubes can interfere with the fertilization process and embryo transport. However, assisted reproductive technologies (ART) such as in vitro fertilization (IVF) can offer viable options for pregnancy in women with hydrosalpinx. In such cases, the fluid-filled tubes are often surgically removed or bypassed to increase the chances of successful implantation.
Q: Can hydrosalpinx be cured without surgery?
A: No, hydrosalpinx typically requires surgical intervention for effective treatment. The accumulation of fluid in the fallopian tubes cannot be resolved without addressing the underlying blockage or damage. While conservative management approaches like antibiotics can help manage associated infections, surgery remains the primary method to address the condition.
Q: What is the main cause of hydrosalpinx?
A: The primary cause of hydrosalpinx is usually pelvic inflammatory disease (PID), which commonly results from sexually transmitted infections (STIs) such as chlamydia or gonorrhea. These infections can cause inflammation and scarring in the fallopian tubes, leading to blockage and the subsequent accumulation of fluid.
Q: Can hydrosalpinx be cancerous?
A: Hydrosalpinx itself is not considered cancerous. It is primarily a structural and functional issue affecting the fallopian tubes. However, it’s important to note that chronic inflammation and certain underlying conditions, such as endometriosis, may increase the risk of developing certain types of ovarian cancer. Regular medical follow-ups and appropriate management are essential to monitor and address any potential risks.
Q: What is the result of hydrosalpinx?
A: Hydrosalpinx can have various outcomes depending on the individual. If left untreated, it can lead to persistent pelvic pain, infertility or difficulty conceiving naturally, and an increased risk of ectopic pregnancy. Treating hydrosalpinx through surgery or assisted reproductive technologies (ART) can improve the chances of successful pregnancy and alleviate associated symptoms.
Q: Is hydrosalpinx an emergency?
A: Hydrosalpinx itself is not typically considered a medical emergency. However, if a hydrosalpinx causes severe pain, signs of infection, or complications such as a ruptured fallopian tube, it may require immediate medical attention. It is important to consult with a healthcare professional for appropriate evaluation and management.
Q: What is the recovery time for hydrosalpinx?
A: The recovery time for hydrosalpinx surgery can vary depending on the surgical approach, individual factors, and any complications. In general, laparoscopic surgery for hydrosalpinx typically involves a shorter recovery period compared to open surgery. Recovery times can range from a few days to a few weeks. It’s important to follow post-operative instructions provided by the healthcare provider and attend any recommended follow-up appointments.
Q: How much does hydrosalpinx surgery cost?
A: The cost of hydrosalpinx surgery can vary depending on various factors, including the geographical location, healthcare facility, surgeon’s fees, type of surgery (laparoscopic or open), additional procedures performed, and insurance coverage. It is recommended to consult with healthcare providers and insurance companies to obtain accurate cost estimates specific to individual circumstances.
Q: Can laparoscopy cure hydrosalpinx?
A: Laparoscopy can be an effective treatment for hydrosalpinx in many cases. During laparoscopic surgery, the fallopian tubes can be assessed and treated by either removing the affected tube (salpingectomy) or creating an opening to drain the fluid (salpingostomy). However, the success of the procedure depends on individual factors, such as the extent of damage and the overall reproductive health of the individual.
Q: Is IVF success possible with hydrosalpinx?
A: In vitro fertilization (IVF) can offer viable options for pregnancy in individuals with hydrosalpinx. Since the fallopian tubes are bypassed during IVF, the blockage or damage caused by hydrosalpinx does not hinder the fertilization process. Prior to IVF, surgical intervention to remove or bypass the affected fallopian tubes may be recommended to increase the chances of successful implantation and pregnancy.
Q: Can hydrosalpinx cause heavy periods?
A: Hydrosalpinx itself typically does not cause heavy periods. However, underlying conditions such as endometriosis, which may coexist with hydrosalpinx, can cause heavy or prolonged menstrual bleeding. If heavy periods are a concern, it is important to consult with a healthcare professional for proper evaluation and diagnosis.
Q: Can hydrosalpinx be seen on ultrasound?
A: Yes, hydrosalpinx can often be visualized on ultrasound. An ultrasound examination can detect the presence of fluid-filled fallopian tubes, which is indicative of hydrosalpinx. Ultrasound is a commonly used imaging modality to assess the reproductive organs and identify structural abnormalities such as hydrosalpinx.