PCOS Tests You Should Know About to Detect & Diagnose PCOS
What is PCOS?
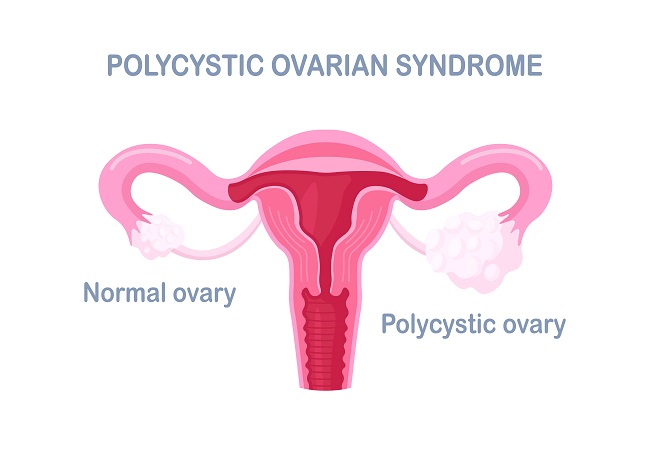
Polycystic Ovary Syndrome (PCOS) is a type of hormonal disorder caused due to excess male sex hormones in females. It’s like an uninvited guest that can wreak havoc on a woman’s life, causing irregular periods, excessive hair growth, acne, and more. But don’t worry, we’re here to help you understand this condition and identify the signs that may indicate you have PCOS. So, let’s dive right into PCOS tests, symptoms, diagnosis & treatment!
PCOS Symptoms: How Do I Know If I Have PCOS?
PCOS can manifest differently in each woman, making it tricky to diagnose. However, there are some common PCOS symptoms that may indicate you have this condition. Let’s take a closer look at them.
- Irregular Periods: One of the most telling signs of PCOS is irregular periods. Does your period come and go like an unpredictable house guest? If so, you may want to consider getting checked for PCOS. Women with this condition often have fewer than eight periods per year or experience long gaps between cycles.
- Excessive Hair Growth (Hirsutism): Have you ever looked in the mirror and wondered why you have more hair on your face, chest, or back than you think you should? This excessive hair growth, called hirsutism, is another common symptom of PCOS. It’s caused by an increase in androgens, the male hormones present in women’s bodies.
- Acne and Oily Skin: Remember those dreaded teenage years when your skin seemed to rebel against you? For some women, acne and oily skin are constant companions, even into adulthood. These unwelcome blemishes may be caused by PCOS, which can lead to an overproduction of sebum (oil) in the skin.
- Thinning Hair or Hair Loss: While some women with PCOS may experience excessive hair growth, others may find their hair thinning or even falling out. This hair loss can be distressing, but it’s essential to remember that you’re not alone. Many women with PCOS struggle with this issue, and finding the right treatment can help.
- Weight Gain and Difficulty Losing Weight: Does it feel like you’re constantly fighting an uphill battle to lose weight? PCOS could be the culprit behind your struggles. Insulin resistance, a common issue in women with PCOS, can make it challenging to shed those extra pounds. But don’t lose hope – with the right treatment plan, you can conquer this challenge.
- Darkening of Skin in Certain Areas: Are you noticing dark patches on your skin, particularly in areas like the neck, groin, or under the breasts? This darkening, known as acanthosis nigricans, may be a sign of PCOS. While it might be tempting to dismiss these changes as harmless, they could be indicative of a more significant issue at play.
- Skin Tags: Another sign of PCOS that you may not have expected is the presence of skin tags. These small, fleshy growths are often found in areas where skin rubs together, such as the neck, armpits, or groin. While skin tags themselves are harmless, their presence could be a clue that your body is experiencing a hormonal imbalance.
Don’t Ignore the Signs: Take Action Today
Now that you’re familiar with the symptoms of PCOS, you’re better equipped to recognize the PCOS first signs in yourself or someone you care about. If you suspect that you or a loved one may have PCOS, don’t hesitate to consult a healthcare professional. Early diagnosis and treatment can make a world of difference in managing this condition and improving your quality of life.
Types of PCOS Tests:
Diagnosing PCOS isn’t as simple as taking a single test. Instead, healthcare professionals use a combination of assessments to get a complete picture of your health. Here’s an overview of the most common tests used in the diagnosis of PCOS.
1. Blood Tests
Blood tests play a significant role in evaluating PCOS. They provide crucial information about the hormone levels, glucose levels, and cholesterol and lipid levels in your body. Let’s take a closer look at these tests.
- Hormone Levels: PCOS is primarily a hormonal disorder, making it essential to evaluate hormone levels. A blood test can measure hormones like luteinizing hormone (LH), follicle-stimulating hormone (FSH), androgens, and more. By analyzing these levels, healthcare professionals can determine if there’s an imbalance that may be causing PCOS symptoms.
- Glucose Levels: Did you know that insulin resistance is a common issue for women with PCOS? A blood test can measure glucose levels to assess if you’re experiencing insulin resistance or are at risk for developing type 2 diabetes.
- Cholesterol and Lipid Levels: Women with PCOS often have higher cholesterol and lipid levels, which can increase the risk of heart disease. A blood test can provide insight into your cardiovascular health and help your healthcare provider develop an appropriate treatment plan.
2. Pelvic Exam
A pelvic exam is another vital step in the PCOS diagnostic process. During this examination, your healthcare provider will assess your reproductive organs for any abnormalities, such as enlarged ovaries or cysts, that might be indicative of PCOS.
3. Ultrasound
An ultrasound is a non-invasive imaging technique that allows healthcare professionals to get a closer look at your ovaries. Let’s explore the two types of ultrasounds used in PCOS diagnosis: transvaginal and abdominal ultrasounds.
Transvaginal Ultrasound: A transvaginal ultrasound involves inserting a probe into the vagina to get a detailed view of the ovaries and uterus. This test can help identify the presence of multiple cysts, a common feature of PCOS.
Abdominal Ultrasound: In some cases, an abdominal ultrasound may be used to assess the ovaries. During this test, a probe is placed on the abdomen to capture images of the reproductive organs. While not as detailed as transvaginal ultrasound, it can still provide valuable information for diagnosing PCOS.
4. Endometrial Biopsy
Although not routinely used in PCOS diagnosis, an endometrial biopsy might be recommended in specific cases. This procedure involves collecting a small sample of tissue from the lining of the uterus to check for abnormalities. An endometrial biopsy can help rule out other conditions that may be causing similar symptoms to PCOS.
PCOS Causes: The Perfect Storm of Factors
PCOS is a multifaceted condition, and several factors can contribute to its development. Let’s take a closer look at these causes and how they intertwine to create the perfect storm for PCOS.
- Genetic Factors: Ever wonder why some families seem more prone to PCOS? The answer lies in their genes. Research suggests that there’s a strong genetic component to PCOS, with a higher likelihood of developing the condition if a close family member has it. However, the exact genes responsible for PCOS are still under investigation.
- Insulin Resistance: Insulin resistance is a common issue in women with PCOS. When the body becomes resistant to insulin, it struggles to effectively process glucose, leading to higher insulin levels. These elevated insulin levels can then trigger the ovaries to produce more androgens, creating a hormonal imbalance and contributing to PCOS symptoms.
- Inflammation: Did you know that inflammation can play a role in PCOS? Women with this condition often have higher levels of inflammation, which can further exacerbate insulin resistance and androgen production. Addressing inflammation is a crucial aspect of managing PCOS.
- Hormonal Imbalances: At the heart of PCOS lies hormonal imbalances. Women with PCOS often have higher levels of androgens, which can disrupt the menstrual cycle, cause excessive hair growth, and contribute to other symptoms. Additionally, imbalances in hormones such as estrogen and progesterone can further complicate the condition.
- Environmental Factors and Lifestyle: Last but not least, environmental factors and lifestyle choices can also contribute to the development of PCOS. Poor diet, lack of exercise, and exposure to environmental toxins can all increase the risk of developing PCOS or worsen existing symptoms.
PCOS Diagnosis:
Now that we understand the causes of PCOS, let’s discuss the importance of accurate PCOS diagnosis and the role of a thorough medical evaluation.
Criteria for Diagnosis
Diagnosing PCOS can be challenging due to the diverse range of symptoms and the absence of a single definitive test. Healthcare professionals typically use the Rotterdam criteria, which require the presence of at least two of the following three features for a diagnosis: irregular periods, elevated androgen levels, and the presence of polycystic ovaries on ultrasound.
Ruling Out Other Conditions
One of the challenges in diagnosing PCOS is that its symptoms can overlap with other medical conditions. A thorough medical evaluation is essential to rule out conditions such as thyroid disorders, adrenal gland disorders, and Cushing’s syndrome. Only by eliminating these possibilities can healthcare professionals accurately diagnose PCOS and develop an appropriate treatment plan.
Importance of a Thorough Medical Evaluation
A comprehensive medical evaluation is crucial for diagnosing PCOS. This process typically involves a detailed medical history, physical examination, blood tests, and imaging studies. By gathering as much information as possible, healthcare professionals can make an informed diagnosis and create a tailored treatment plan to address your unique needs.
PCOS Treatment:
To Cure PCOS permanently you must follow:
- Lifestyle Changes: Before diving into medications and surgical options, let’s discuss the power of lifestyle changes in managing PCOS. Embracing a healthy lifestyle can significantly impact your symptoms and overall well-being.
- Diet: A balanced diet is crucial in managing PCOS. Focus on whole foods, and whole grains, such as fruits, vegetables, and lean proteins. Additionally, it’s essential to limit processed foods and added sugars. Eating a balanced diet can help regulate insulin levels, reduce inflammation, and promote weight loss, which can all improve PCOS symptoms.
- Exercise: Did you know that regular exercise can work wonders for PCOS? Engaging in physical activity can help lower insulin levels, manage weight, and alleviate stress. Do at least 150 minutes of moderate-intensity PCOS exercise per week, incorporating both cardio and strength training for optimal results.
- Stress Management: Stress can exacerbate PCOS symptoms, making it essential to find effective stress management techniques. Meditation, yoga, deep breathing exercises, and spending time in nature are all great ways to manage stress and promote overall well-being.
PCOS Medications:
In some cases, lifestyle changes may not be enough to manage PCOS symptoms. That’s where medications come in! There are several medication options available to target specific PCOS symptoms.
- Hormonal Contraceptives: Hormonal contraceptives, such as birth control pills, can help regulate menstrual cycles, reduce excessive hair growth, and clear acne by balancing hormone levels.
- Anti-Androgen Medications: Anti-androgen medications can help reduce excessive hair growth and acne by blocking the effects of androgens, a group of hormones that can contribute to PCOS symptoms.
- Insulin-Sensitizing Drugs: Insulin-sensitizing drugs, such as metformin, can help improve insulin resistance, regulate menstrual cycles, and promote weight loss in women with PCOS.
- Fertility Treatments: If you’re trying to conceive, fertility treatments like clomiphene citrate or gonadotropin injections can help stimulate ovulation and increase the chances of becoming pregnant.
- Surgery: In some cases, surgical intervention may be necessary to manage PCOS symptoms, particularly when other treatments have been unsuccessful.
- Ovarian Drilling: Ovarian drilling is a minimally invasive procedure in which small holes are made in the ovaries to reduce androgen production. This surgery can help restore regular ovulation and improve fertility in some women with PCOS.
- Weight Loss Surgery (in Select Cases): Weight loss surgery, such as gastric bypass or sleeve gastrectomy, may be considered in select cases where obesity significantly contributes to PCOS symptoms and other treatments have failed. This option should only be considered after a thorough evaluation by a healthcare professional.
Personalizing Your PCOS Treatment Plan with Little Angel IVF
Remember, there’s no one-size-fits-all approach to PCOS treatment. It’s essential to work closely with your healthcare provider to develop a personalized plan tailored to your unique needs and goals. By combining lifestyle changes, medications, and, if necessary, surgical interventions, you can regain control of your life and successfully manage PCOS.
Conclusion
Understanding the various types of PCOS tests and their role in diagnosing this complex condition is essential for anyone affected by or suspecting they have PCOS. Early diagnosis and intervention can significantly improve the management of symptoms and overall quality of life. Remember, you are not alone in your journey, and knowledge is power. By arming yourself with information about PCOS tests and working closely with your healthcare provider, you can take control of your health and embark on the path to a brighter, healthier future.
F.A.Q
Q: What tests are done to confirm PCOS?
A: PCOS can be confirmed through a combination of medical history, physical examination, and tests such as blood tests, ultrasound, and hormone tests.
Q: How can I test PCOS at home?
A: There are no home tests available to diagnose PCOS.
Q: How will I know if I have PCOS?
A: Symptoms of PCOS may include irregular periods, excessive hair growth, acne, weight gain, and difficulty getting pregnant. A healthcare provider can perform tests and diagnose PCOS.
Q: What is the cost of the PCOD test?
A: The cost of PCOS testing may vary depending on the healthcare provider and the type of tests performed.
Q: What hormones are tested for PCOS?
A: Hormones commonly tested for PCOS include luteinizing hormone (LH), follicle-stimulating hormone (FSH), testosterone, and insulin.
Q: Can PCOS get pregnant?
A: PCOS can make it difficult to conceive, but many women with PCOS are able to become pregnant with proper treatment.
Q: When is the best time for a PCOS test?
A: It is best to have PCOS testing performed when you are experiencing symptoms such as irregular periods, excessive hair growth, and weight gain.
Q: Can PCOD be cured?
A: PCOS cannot be cured, but it can be managed through lifestyle changes, medication, and other treatments.
Q: Can a urine test detect PCOS?
A: No, a urine test cannot detect PCOS. PCOS is diagnosed through medical history, physical examination, and tests such as blood tests, ultrasound, and hormone tests.
Q: Is PCOS a serious problem?
A: PCOS is a chronic condition that can lead to serious health problems such as diabetes, heart disease, and infertility if left untreated.
Q: At what age does PCOS start?
A: PCOS can start at any age after puberty, but it is most commonly diagnosed in women in their 20s or 30s.
Q: What does a PCOS belly look like?
A: PCOS can cause weight gain, particularly in the abdominal area, which can lead to a “potbelly” appearance.
Q: Can you have PCOS with regular periods?
A: Yes, it is possible to have PCOS with regular periods. However, irregular periods are just common symptoms of PCOS.
Q: What is the difference between PCOD and PCOS?
A: PCOD (polycystic ovary disease) and PCOS (polycystic ovary syndrome) are often used interchangeably, but PCOS is a more accurate term as it encompasses a broader range of symptoms beyond just cysts on the ovaries.
Q: How long can PCOS delay your period?
A: PCOS can cause irregular periods or even missed periods, but the length of delay can vary from person to person.
Q: Should I see a gynecologist or endocrinologist for PCOS?
A: Both gynecologists and endocrinologists can diagnose and treat PCOS, but it is recommended to seek care from a healthcare provider with experience in treating the condition.
