MRKH Syndrome: Symptoms, Causes & Treatment
What Is MRKH Syndrome?
Imagine a puzzle where one critical piece is missing, preventing the completion of the picture. MRKH syndrome can be likened to such a puzzle. Mayer-Rokitansky-Küster-Hauser syndrome, often referred to as MRKH- syndrome or simply MRKH, is a rare condition that affects the development of a woman’s reproductive system during fetal growth. It is estimated to occur in approximately 1 in 4,000 women worldwide, emphasizing the significance of shedding light on this condition.
Types of MRKH Syndrome
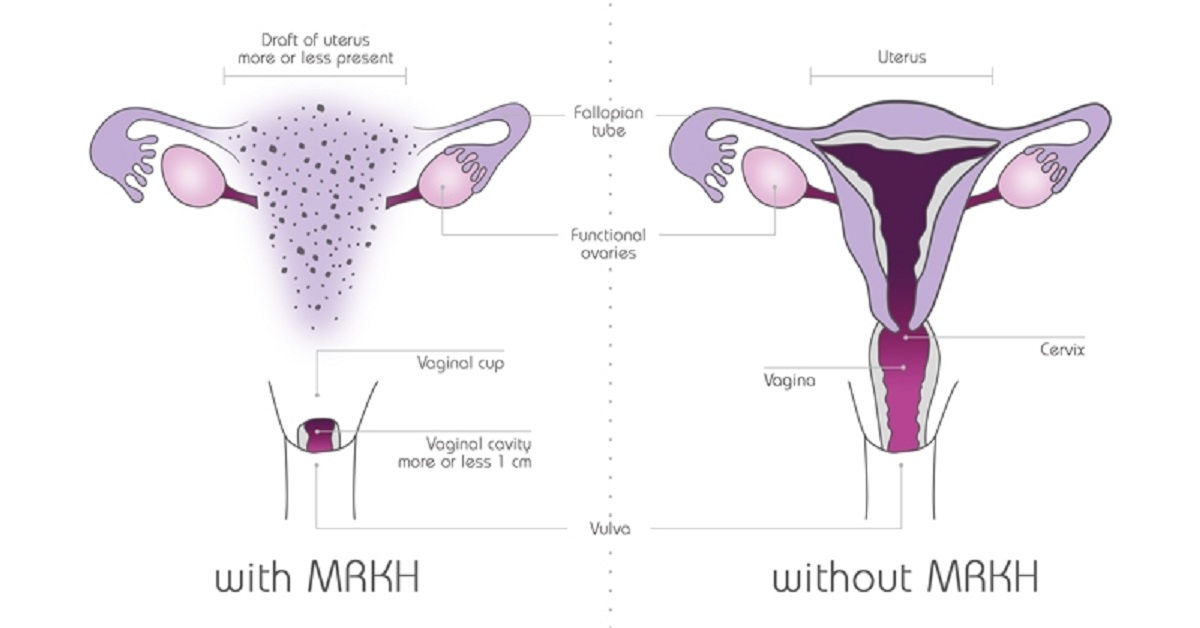
Type 1 MRKH -Syndrome: Type 1 MRKH syndrome is the most common form of the condition. In this type, the uterus is either partially or completely absent, while the ovaries and fallopian tubes typically develop normally. It is important to note that individuals with type 1 MRKH syndrome have functional ovaries and can produce eggs. However, due to the absence of the uterus, natural conception and carrying a pregnancy to term is not possible.
Type 2 MRKH -Syndrome: Type 2 MRKH syndrome is characterized by the absence of the uterus, similar to type 1. However, individuals with type 2 MRKH syndrome may also experience additional reproductive system anomalies. These anomalies can include abnormalities in the vagina, cervix, fallopian tubes, and/or the kidneys. The severity and combination of these additional anomalies may vary from person to person.
Symptoms of MRKH Syndrome:
While MRKH syndrome primarily affects the reproductive system, its impact extends far beyond the physical aspect. The emotional journey experienced by individuals with MRKH syndrome can be challenging and filled with various emotions. Understanding the symptoms and providing support is crucial for both patients and their loved ones.
- Absence of Menstruation: The absence of menstruation, also known as primary amenorrhea, is often the first indication of MRKH syndrome. During adolescence, when girls typically begin menstruating, those with MRKH syndrome do not experience this milestone. This revelation can be met with shock, confusion, and a sense of feeling “different” from their peers.
- Difficulty with Sexual Intercourse: Another symptom experienced by individuals with MRKH syndrome is difficulty with sexual intercourse. Due to the underdevelopment of the vagina, intercourse can be painful or even impossible. This can lead to feelings of frustration, inadequacy, and a strain on intimate relationships.
- Emotional Impact: The emotional impact of MRKH syndrome should not be underestimated. The diagnosis can evoke feelings of grief and loss as individuals process the news of their reproductive challenges. Questions about identity, femininity, and future motherhood may arise, causing emotional distress. It is important to provide emotional support and create a safe space for individuals with MRKH syndrome to express their feelings and concerns.
Causes MRKH Syndrome :
- Genetic Factors: Genetics may play a pivotal role in MRKH syndrome. Research suggests that certain genetic abnormalities and mutations could contribute to the development of this condition. However, it’s important to note that MRKH syndrome is not typically inherited from parents. Rather, it is considered a sporadic occurrence, arising from random genetic events during fetal development.
- Embryological Factors: Embryological factors are believed to contribute to MRKH syndrome. During early embryonic development, the Müllerian ducts, which give rise to the uterus, fallopian tubes, and upper vagina, may fail to develop properly or undergo incomplete fusion. This developmental anomaly leads to the characteristic features observed in individuals with MRKH syndrome.
- Environmental Factors: While the role of environmental factors in MRKH syndrome is not yet fully understood, it is believed that certain environmental influences during fetal development may contribute to the condition. Exposure to certain toxins, infections, or hormonal imbalances in the womb could potentially disrupt normal reproductive system development, leading to MRKH syndrome.
Diagnosis of MRKH Syndrome:
Reaching a diagnosis of MRKH syndrome is a crucial step in understanding and managing the condition. A comprehensive diagnostic process involves various medical evaluations and tests.
- Medical History and Physical Examination: When seeking a diagnosis for MRKH at Little Angel IVF, your healthcare provider will begin by taking a detailed medical history and conducting a thorough physical examination. This allows them to gather essential information about your menstrual history, sexual development, and any other relevant symptoms or conditions.
- Imaging Studies: Imaging studies, such as pelvic ultrasound and magnetic resonance imaging (MRI), play a significant role in diagnosing MRKH syndrome. These non-invasive procedures provide detailed images of the reproductive organs, helping to identify any structural abnormalities or the absence of the uterus and upper vagina.
- Chromosomal Analysis: Chromosomal analysis, commonly known as karyotyping, may be performed to rule out other genetic disorders and assess the chromosomal makeup of individuals with MRKH syndrome. Although MRKH syndrome is not typically caused by chromosomal abnormalities, this test helps to ensure a comprehensive evaluation.
- Laparoscopy: In some cases, laparoscopy may be recommended to further investigate the reproductive anatomy. During this minimally invasive surgical procedure, a thin tube with a camera is inserted through small incisions in the abdomen, allowing for direct visualization of the pelvic organs and confirmation of the diagnosis.
Treatment for MRKH Syndrome:
Surgical interventions play a key role in the management of MRKH syndrome. The primary goal of surgery is to create a neovagina, a surgically constructed vaginal canal. Different surgical techniques, such as the McIndoe procedure or the Vecchietti technique, may be employed to achieve this. These procedures involve creating a vaginal canal using tissue grafts or non-surgical techniques like dilator therapy.
Prevention of MRKH Syndrome:
Preventing MRKH syndrome is a complex challenge due to its multifactorial nature. However, gaining insights into potential risk factors and understanding preventive measures can contribute to overall reproductive health.
- Genetic Counseling: Genetic counseling plays a vital role in understanding the risk factors associated with MRKH. Individuals with a family history of MRKH or related conditions may benefit from genetic counseling to assess the likelihood of passing on the syndrome to future generations. By gaining a deeper understanding of the condition and its potential genetic implications, individuals can make informed decisions about family planning.
- Early Detection: While MRKH syndrome is typically diagnosed during adolescence or early adulthood, early detection can facilitate timely intervention and emotional support. Raising awareness among healthcare professionals about the signs and symptoms of MRKH syndrome can aid in early diagnosis and improve outcomes for individuals.
Diet in MRKH Syndrome:
Maintaining a healthy diet is essential for overall well-being, and it can play a supportive role in managing MRKH syndrome. Although there are no specific dietary guidelines exclusive to MRKH syndrome, adopting a balanced approach can promote optimal health.
- Nutrient-Rich Foods: Including a variety of nutrient-rich foods in your diet is beneficial for individuals with MRKH syndrome. Focus on consuming a balanced mix of fruits, vegetables, whole grains, lean proteins, and healthy fats. These foods provide essential vitamins, minerals, and antioxidants that support overall health and well-being.
- Adequate Hydration: Staying adequately hydrated is crucial for everyone, including individuals with MRKH. Water helps maintain proper bodily functions and supports overall health. Aim to drink an adequate amount of water throughout the day to keep your body hydrated and promote optimal functioning.
- Mindful Eating: Practicing mindful eating can be beneficial for individuals with MRKH syndrome. Take time to savor and appreciate your meals, paying attention to hunger and fullness cues. Engage all your senses while eating, focusing on the flavors, textures, and enjoyment of the food. This mindful approach can help foster a positive relationship with food and promote overall well-being.
- Consulting a Registered Dietitian: For individuals with specific dietary concerns or questions, consulting a registered dietitian can provide personalized guidance. A dietitian can assess your individual needs, help develop a tailored meal plan, and address any nutritional concerns you may have. They can also provide support in managing any comorbid conditions that may be present alongside MRKH syndrome.
Also Read :- Top 10 Best IVF Centre in Delhi with High Success Rates
Conclusion:
Mayer-Rokitansky-Küster-Hauser (MRKH) syndrome poses unique challenges to women’s reproductive health. However, through understanding, support, and access to access to specialized care at Little Angel IVF, individuals with MRKH can thrive and lead fulfilling lives. Surgical interventions, emotional support, and preventive measures contribute to a holistic approach to managing this condition. Additionally, adopting a nourishing diet can support overall well-being and promote optimal health.
F.A.Q
Q: What does MRKH syndrome look like?
A: MRKH syndrome, also known as Mayer-Rokitansky-Küster-Hauser syndrome, does not have any physical manifestations that can be visually identified. It is a congenital condition that primarily affects the reproductive system in females.
Q: Do people with MRKH have periods?
A: No, individuals with MRKH syndrome do not have periods. One of the main characteristics of MRKH syndrome is the absence or underdevelopment of the uterus, which is responsible for menstruation.
Q: What is the cause of MRKH syndrome?
A: The exact cause of MRKH syndrome is currently unknown. It is believed to be a result of a combination of genetic and environmental factors, but no specific cause has been identified thus far.
Q: How is MRKH syndrome diagnosed?
A: MRKH syndrome is typically diagnosed through a series of medical evaluations and tests. These may include a physical examination, pelvic ultrasound, imaging tests (such as MRI or CT scan), and genetic testing. A thorough medical history is also taken into account during the diagnostic process.
Q: Do you produce eggs with MRKH?
A: Yes, individuals with MRKH syndrome typically have functioning ovaries and are capable of producing eggs (ova). However, due to the absence or underdevelopment of the uterus and upper vaginal canal, natural conception and pregnancy are not possible without medical intervention.
Q: Do girls with MRKH ovulate?
A: Yes, girls with MRKH syndrome typically experience ovulation, which is the release of an egg from the ovary. However, as mentioned earlier, the absence or underdevelopment of the uterus and upper vaginal canal prevents natural conception and pregnancy without medical assistance.
Q: Is there a cure for MRKH?
A: Currently, there is no cure for MRKH syndrome. However, various treatments and interventions are available to address the specific challenges associated with the condition. These may include surgical options to create a neovagina (a new vaginal canal) or assisted reproductive technologies (such as in vitro fertilization) to facilitate pregnancy.
Q: Can a woman get pregnant without a uterus?
A: In general, a woman cannot become pregnant without a uterus. The uterus is the organ where a fertilized egg implants and develops into a fetus. However, in cases of MRKH syndrome or other conditions where the uterus is absent or nonfunctional, alternative options such as surrogacy or adoption can be considered for individuals who desire to have children.
Q: Is there a male version of MRKH?
A: No, MRKH syndrome is exclusive to individuals assigned to females at birth. However, there are other congenital conditions that can affect the reproductive system in males, such as androgen insensitivity syndrome (AIS) or congenital absence of the vas deferens (CAVD).
Q: Can MRKH syndrome be cured?
A: MRKH syndrome cannot be completely cured since it is a congenital condition. However, various treatments and interventions can help manage the challenges associated with MRKH, such as creating a functional neovagina or exploring assisted reproductive technologies to achieve pregnancy. The goal of these interventions is to improve the quality of life and reproductive options for individuals with MRKH syndrome.