Effects of Bicornuate Uterus on Pregnancy & Its Treatment
What is a Bicornuate Uterus?
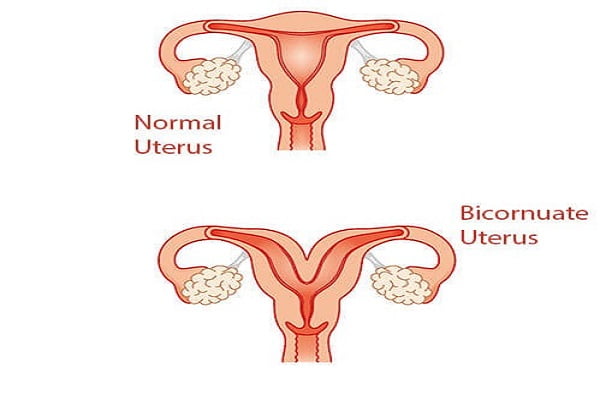
A bicornuate uterus is an unusual congenital uterine malformation characterized by a heart-shaped uterus with a deep indentation at the top. This abnormality occurs due to the incomplete fusion of the two Müllerian ducts during fetal development. As a result, the uterus develops with two separate cavities instead of one single cavity.
Having a bicornuate uterus does not necessarily mean that a woman will face fertility issues or pregnancy complications. Many women with this condition go on to have healthy pregnancies and deliver healthy babies. However, in some cases, it can cause complications, such as an increased risk of miscarriage, preterm labor, or malpresentation of the baby.
Types of Bicornuate Uterus:
There are two primary types of bicornuate uterus, each with its unique characteristics and implications for pregnancy:
- Partial Bicornuate Uterus; In a partial bicornuate uterus, the indentation at the top of the uterus is not as deep, and the two cavities are partially fused. This type of bicornuate uterus is less likely to cause pregnancy complications than a complete bicornuate uterus.
- Complete Bicornuate Uterus: A complete bicornuate uterus has a deeper indentation at the top, resulting in two distinct and separate cavities. This type of bicornuate uterus poses a higher risk for pregnancy complications, such as miscarriage or preterm labor.
Also Read: Uterus Meaning in Hindi
What are the Causes of Bicornuate Uterus?
Researchers have not yet been able to pinpoint the exact cause of bicornuate uterus, but there are two main factors that are believed to play a role in its development: genetic factors and environmental factors.
- Genetic Factors: Genetic factors can predispose a woman to have a bicornuate uterus. It is thought that certain genes might influence the development of the Müllerian ducts, which, in turn, determine the shape of the uterus. However, more research is needed to identify the specific genes involved and how they might interact with other factors to cause this condition.
- Environmental Factors; Environmental factors can also play a role in the development of a bicornuate uterus. Some studies suggest that exposure to certain chemicals or substances during pregnancy might interfere with the normal development of the uterus. For example, a pregnant woman’s exposure to diethylstilbestrol (DES), a synthetic estrogen used from the 1940s to the 1970s, has been linked to an increased risk of uterine malformations in their daughters.
In addition, factors such as maternal illness, stress, or exposure to radiation during pregnancy might also contribute to the development of a bicornuate uterus. However, it is essential to keep in mind that the exact relationship between these factors and the condition is not yet fully understood, and more research is needed to establish a clear link.
Symptoms of Bicornuate Uterus:
A bicornuate uterus may present no noticeable symptoms in many women, making it challenging to diagnose. However, some women may experience symptoms that indicate the presence of this condition.
Common Symptoms
Some of the most common symptoms associated with a bicornuate uterus include:
- Irregular menstrual cycles: Women with a bicornuate uterus may experience irregular or heavy periods, sometimes accompanied by severe cramping.
- Recurrent miscarriages: A bicornuate uterus can increase the risk of miscarriages, especially during the first trimester of pregnancy.
- Infertility: Difficulty conceiving can be another sign of a bicornuate uterus, as the abnormal shape of the uterus may interfere with the implantation of a fertilized egg.
How Symptoms May Vary
It’s important to note that not all women with a bicornuate uterus will experience the same symptoms or face the same challenges. Some women may have mild symptoms or no symptoms at all, while others may have more severe or persistent symptoms. The severity of symptoms and the impact on fertility can vary based on the degree of uterine malformation.
Also Read: Bulky Uterus In Hindi
Diagnosis of Bicornuate Uterus
If you suspect you may have a bicornuate uterus due to the presence of the symptoms mentioned above or a family history of uterine malformations, it is crucial to consult a healthcare professional for a proper diagnosis. Here are some of the methods used to diagnose a bicornuate uterus:
- Physical Examination: A healthcare provider may perform a pelvic examination to assess the size and shape of the uterus. While this examination can provide some information, it may not be sufficient to confirm the presence of a bicornuate uterus, as the abnormality might not be easily felt during a physical examination.
- Imaging Techniques: To obtain a more detailed and accurate picture of the uterus, healthcare professionals may use imaging techniques such as:
- Ultrasound: Ultrasound is often the first diagnostic tool used to assess the shape and structure of the uterus. This non-invasive method uses sound waves to create images of the pelvic organs, allowing the healthcare provider to identify any abnormalities in the uterus.
- MRI: Magnetic resonance imaging (MRI) is another imaging method that can provide more detailed images of the uterus. An MRI uses powerful magnets and radio waves to create detailed images of the body’s internal structures. This method can be particularly helpful in determining the extent of the uterine malformation and differentiating a bicornuate uterus from other uterine abnormalities.
- Diagnostic Laparoscopy: In some cases, healthcare providers may recommend a diagnostic laparoscopy to confirm the presence of a bicornuate uterus. This minimally invasive surgical procedure involves the insertion of a small camera through a tiny incision in the abdomen, allowing the surgeon to examine the pelvic organs directly. While this method is more invasive than imaging techniques, it can provide a definitive diagnosis and help guide treatment decisions.
Effects of Bicornuate Uterus on Pregnancy:
A bicornuate uterus can impact various aspects of pregnancy, from conception to delivery. Let’s take a closer look at some of the challenges women with this condition may encounter.
- Fertility and Conception: While a bicornuate uterus doesn’t always cause fertility issues, it can make conception more difficult for some women. The abnormal shape of the uterus can hinder the implantation of a fertilized egg, resulting in challenges in conceiving.
- Pregnancy Complications: A bicornuate uterus can increase the risk of various pregnancy complications, such as:
- Preterm Labor: Women with a bicornuate uterus are at a higher risk of experiencing preterm labor, as the abnormal shape of the uterus may not allow the baby to grow and develop adequately.
- Malpresentation: A bicornuate uterus can also contribute to malpresentation, where the baby is not positioned correctly for a vaginal delivery. This can increase the likelihood of needing a cesarean section.
- Cervical Incompetence: Cervical incompetence, where the cervix begins to dilate prematurely, is another potential complication associated with a bicornuate uterus. This condition can lead to preterm labor and may require medical intervention, such as a cervical cerclage, to help prevent early delivery.
- Miscarriage: Unfortunately, women with a bicornuate uterus are at a higher risk of miscarriage, particularly during the first trimester of pregnancy. This is often due to the abnormal shape of the uterus, which can interfere with the growth and development of the embryo.
Bicornuate Uterus Pregnancy Success Rates in India
While a bicornuate uterus can present challenges, it’s essential to remain hopeful and informed about the possibilities for successful pregnancies.
Statistical Overview
In India, the overall success rate for pregnancies among women with a bicornuate uterus is estimated to be around 60-70%. This means that a significant number of women with this condition can achieve successful pregnancies, despite the increased risks and challenges.
Factors Affecting Success Rates:
Several factors can influence the success rates of pregnancies in women with a bicornuate uterus, including:
- Degree of uterine malformation: Women with a partial bicornuate uterus generally have a higher chance of successful pregnancy compared to those with a complete bicornuate uterus.
- Access to quality healthcare: Timely and appropriate prenatal care, monitoring, and interventions can significantly improve pregnancy outcomes for women with a bicornuate uterus.
- Individual health factors: A woman’s overall health, age, and lifestyle choices can also impact her chances of a successful pregnancy.
While the challenges associated with a bicornuate uterus can be daunting, it’s crucial to remain optimistic and proactive in managing this condition. Regular prenatal care, a healthy lifestyle, and a strong support system can make a world of difference for women with a bicornuate uterus embarking on the journey of motherhood.
Treatment of Bicornuate Uterus:
There are several treatment options available for women with a bicornuate uterus. Let’s delve into some of the most common methods.
- Hysteroscopic Metroplasty: Hysteroscopic metroplasty is a minimally invasive surgical procedure that aims to reshape the uterus. This technique involves using a small camera called a hysteroscope, which is inserted through the cervix to examine the uterus. Your doctor will then use specialized instruments to remove the septum that divides the uterus, helping it to regain a more regular shape.
- Laparoscopic Strassman Metroplasty; Another surgical option is laparoscopic Strassman metroplasty. This procedure is performed through small incisions in the abdomen, using a laparoscope (a thin tube with a camera) for guidance. The surgeon will reshape the uterus, removing the septum and suturing the incisions closed.
- Fertility Treatments: In some cases, fertility treatments such as in-vitro fertilization (IVF) may be recommended for women with a bicornuate uterus who struggle to conceive. IVF can increase the chances of a successful pregnancy by bypassing the potential complications caused by the abnormal uterine shape.
- Preconception Counseling; Preconception counseling is an essential part of treating a bicornuate uterus. This process involves discussing potential risks, complications, and treatment options with your healthcare provider before attempting to conceive. This proactive approach can help you make informed decisions and better prepare for a healthy pregnancy.
Preventing Bicornuate Uterus
While it’s crucial to focus on preventing complications and promoting overall health during pregnancy, it’s important to recognize the limitations in preventing the formation of a bicornuate uterus.
Understanding Limitations in Prevention: A bicornuate uterus is a congenital condition, which means it’s present at birth and develops during the early stages of fetal development. Unfortunately, there are no known ways to prevent the formation of a bicornuate uterus, as it’s likely a result of genetic and environmental factors.
Promoting Healthy Prenatal Development: Although preventing a bicornuate uterus may not be possible, promoting healthy prenatal development is still vital. Expectant mothers can take several steps to ensure a healthy pregnancy, including:
- Maintaining a well-balanced diet
- Taking prenatal vitamins, including folic acid
- Staying active with safe exercises approved by a healthcare provider
- Avoiding exposure to harmful substances, such as alcohol, tobacco, and drugs
- Managing stress and practicing self-care
Health Risks Associated with Bicornuate Uterus:
A bicornuate uterus can present health risks for both the mother and the baby during pregnancy. It’s essential to understand these risks to be better prepared and take necessary precautions.
Maternal Risks: Women with a bicornuate uterus may face several health risks, including:
- Preterm labor: The abnormal shape of the uterus can lead to preterm labor, increasing the risk of complications for both the mother and baby.
- Cesarean section: Due to malpresentation or other complications, women with a bicornuate uterus may require a cesarean section for delivery.
- Cervical incompetence: Cervical incompetence can lead to preterm labor and may require medical intervention to prevent early delivery.
Fetal Risks: Babies born to mothers with a bicornuate uterus may also face specific health risks, such as:
- Growth restrictions: The abnormal shape of the uterus may restrict the baby’s growth, leading to potential complications and the need for close monitoring.
- Premature birth: Preterm labor can result in premature birth, which can present various challenges, including underdeveloped organs and a weakened immune system.
- Congenital anomalies: Some studies suggest that babies born to mothers with a bicornuate uterus may have a slightly increased risk of congenital anomalies, although the overall risk remains low.
Despite the risks associated with a bicornuate uterus, many women with this condition can still have successful pregnancies with the help of appropriate medical care and monitoring. It’s crucial to work closely with a healthcare provider who understands the challenges and risks associated with a bicornuate uterus to ensure the best possible outcome.
Conclusion
Navigating pregnancy with a bicornuate uterus can present unique challenges and risks for both the mother and baby. However, with the right knowledge, support, and medical care, many women with this condition can experience successful pregnancies and healthy outcomes. By understanding the effects of a bicornuate uterus on pregnancy, the potential complications, and the available treatment options, women can make informed decisions and be better prepared for their journey through motherhood. It’s essential to maintain open communication with healthcare providers and seek timely care to optimize the chances of a healthy, successful pregnancy. Remember, you’re not alone in this journey, and with the right resources and support, you can overcome the challenges posed by a bicornuate uterus and embrace the joys of motherhood.
F.A.Q
Q: Can you have a baby with a bicornuate uterus?
A: Yes, many women with a bicornuate uterus can have a baby. However, they may face an increased risk of pregnancy complications, so it’s essential to work closely with a healthcare provider for appropriate monitoring and care.
Q: Is bicornuate uterus high risk?
A: A bicornuate uterus is considered a high-risk pregnancy factor due to the increased likelihood of complications, such as preterm labor, malpresentation, cervical incompetence, and miscarriage. It’s crucial for women with a bicornuate uterus to receive proper prenatal care and monitoring.
Q: What is a normal size bicornuate uterus?
A: A bicornuate uterus varies in size and shape, but it generally has a heart-shaped appearance due to the partial or complete split of the upper part of the uterus. The size of a bicornuate uterus can vary depending on the depth of the cleft and the individual woman’s anatomy.
Q: How is a bicornuate uterus fixed?
A: In some cases, a bicornuate uterus can be surgically corrected through a procedure called metroplasty. This procedure aims to reshape the uterus and create a single uterine cavity, potentially reducing the risk of pregnancy complications. However, not all women with a bicornuate uterus require surgery, and it’s essential to discuss the risks and benefits with a healthcare provider.
Q: Is bicornuate uterus normal?
A: A bicornuate uterus is a congenital uterine malformation that affects a small percentage of women. While it’s not considered “normal,” many women with a bicornuate uterus can still have successful pregnancies with proper care and monitoring.
Q: What are the disadvantages of a bicornuate uterus?
A: Disadvantages of a bicornuate uterus include an increased risk of pregnancy complications such as preterm labor, malpresentation, cervical incompetence, and miscarriage. Women with a bicornuate uterus may also require cesarean sections for delivery.
Q: What position is the baby with a bicornuate uterus?
A: The baby’s position in a bicornuate uterus can vary, but the abnormal shape of the uterus may increase the likelihood of malpresentation, such as breech or transverse presentation. This can lead to complications during labor and may require a cesarean section for delivery.
Q: Does a bicornuate uterus affect periods?
A: A bicornuate uterus does not typically affect the regularity or duration of periods. However, some women with a bicornuate uterus may experience more painful periods due to the uterus’s abnormal shape. If you have concerns about your menstrual cycle, consult your healthcare provider for evaluation and advice.
Q: What is the success rate of pregnancy with a bicornuate uterus?
A: The success rate of pregnancy with a bicornuate uterus can vary depending on individual factors and the degree of the uterine malformation. While there is an increased risk of pregnancy complications, many women with a bicornuate uterus can still have successful pregnancies with proper care and monitoring. The success rate may be higher for those who undergo surgical correction.
Q: What causes a bicornuate uterus?
A: A bicornuate uterus is a congenital uterine malformation caused by incomplete fusion of the Müllerian ducts during embryonic development. The exact cause of this abnormal development is not well understood, but it may involve a combination of genetic and environmental factors.
Q: What degree is bicornuate uterus?
A: The degree of a bicornuate uterus refers to the extent of the cleft dividing the uterine cavity. It can range from a partial cleft, where only the upper part of the uterus is divided, to a complete cleft that extends all the way to the cervix. The degree of the bicornuate uterus can impact pregnancy outcomes and the risk of complications.
Q: What is the best birth control for a bicornuate uterus?
A: The best birth control option for a woman with a bicornuate uterus depends on her individual needs, preferences, and medical history. It’s essential to discuss birth control options with a healthcare provider who can take these factors into account and provide personalized recommendations.
Q: Can a bicornuate uterus be painful?
A: A bicornuate uterus does not typically cause pain on its own. However, some women with a bicornuate uterus may experience more painful periods due to the abnormal shape of the uterus. If you have concerns about pain or discomfort, consult your healthcare provider for evaluation and advice.
Q: Can you carry a child with a heart-shaped uterus?
A: Yes, many women with a heart-shaped uterus, also known as a bicornuate uterus, can carry a child. However, they may face an increased risk of pregnancy complications and should work closely with their healthcare provider to ensure proper care and monitoring during pregnancy.
Q: Can a bicornuate uterus carry twins?
A: While it is possible for a woman with a bicornuate uterus to conceive and carry twins, it may be more challenging due to the increased risk of pregnancy complications. Carrying twins can place additional strain on the uterus and increase the risk of preterm labor, malpresentation, and other issues. It’s essential for women with a bicornuate uterus carrying twins to receive proper prenatal care and monitoring to optimize the chances of a healthy pregnancy.